The Hidden Costs of Inefficient Deliveries in Senior Care Providers
Share this post
Most administrators focus on care ratios, staffing, and compliance. But quietly bleeding money in the background is a problem that rarely makes it onto the...
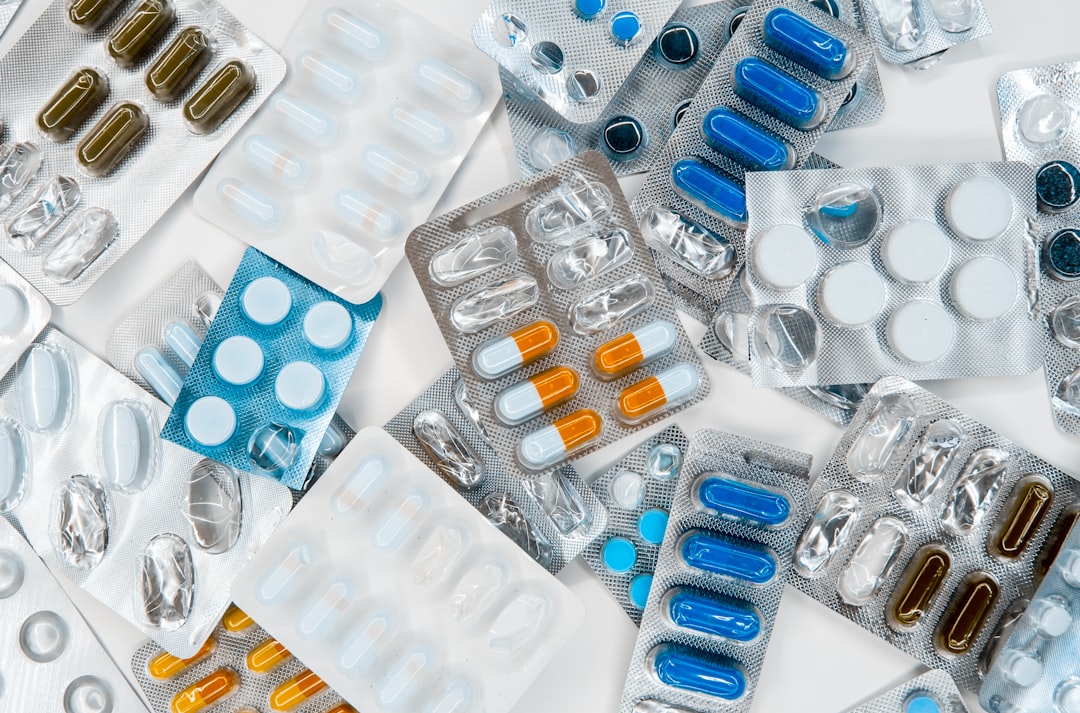
Senior care facilities run on supplies.
Medications, incontinence products, nutritional supplements, wound care materials, medical equipment — the list is endless, and it never stops.
For a mid-sized assisted living facility serving 80–120 residents, that means hundreds of individual deliveries per month, dozens of vendors, and a constant churn of orders, receipts, invoices, and returns.
And most of it is managed on spreadsheets, phone calls, and institutional memory.
The result?
An operational blind spot that costs the average senior care provider between $180,000 and $340,000 per year in direct and indirect losses and most of them don't even know it.
What "Inefficient Deliveries" Actually Costs You
The costs aren't just financial. They ripple outward into care quality, staff morale, regulatory risk, and resident outcomes. Here's where the damage accumulates:
1. Receiving Errors and Shrinkage
When deliveries arrive without proper verification workflows, discrepancies go undetected. Studies in healthcare supply chain management estimate that 3–8% of delivered goods are either wrong, damaged, short-shipped, or never arrive at all — and a significant portion of those discrepancies are never caught, let alone recovered.
For a facility spending $2 million annually on supplies, that's up to $160,000 walking out the door (or never walking in).
2. Staff Time Diverted From Care
When a nurse has to chase a missing delivery, reconcile an invoice against a paper packing slip, or call a vendor to dispute a charge, that's direct care time lost.
The American Health Care Association has found that supply chain administration consumes an average of 4.2 hours per nurse per week in facilities without automated systems.
At 30 nursing staff, that's over 6,500 hours per year — the equivalent of more than three full-time employees — spent on logistics paperwork instead of residents.
3. Emergency Purchasing Premiums
Stockouts happen. When a critical supply runs out because nobody caught a short delivery or a missed order, the facility scrambles.
Emergency purchasing from secondary vendors typically costs 15–40% more than contracted rates, and expedited shipping adds further.
A single missed pallet of wound care supplies can cost a 150-bed facility thousands in emergency procurement — and it happens regularly.
4. Invoice Disputes and Billing Leakage
Without digital proof of delivery — timestamped, geo-verified, signed — disputing a vendor invoice is nearly impossible. Facilities routinely pay for goods they didn't receive simply because they can't prove the absence.
Conservative industry estimates put unrecovered billing discrepancies at 2–4% of total supply spend across the sector.
5. Compliance and Audit Exposure
State surveyors and federal auditors require facilities to demonstrate proper medication delivery chains, controlled substance receipt verification, and supply chain traceability. Facilities operating on paper or fragmented systems face citation risk.
A single deficiency related to medication delivery documentation can trigger a plan of correction, increased survey frequency, and reputational damage that affects occupancy.
6. Resident Outcomes and Quality Scores
This is the one that keeps administrators up at night. When supplies are delayed or missing — a resident's specific nutritional formula, a specialized wound dressing, a scheduled medication — care is compromised.
Beyond the human cost, quality measure scores drop, star ratings suffer, and referral pipelines dry up.
A one-star drop on CMS ratings is associated with occupancy declines of 5–8%, which for a 120-bed facility at $6,000/month average rate represents over $400,000 in annualized revenue at risk.
The Compounding Problem Nobody Measures
Here's the insidious part: these costs don't show up cleanly on any single line item. The emergency purchasing premium hides in the supplies budget.
The lost staff time hides in payroll. The unrecovered billing discrepancies are invisible because nobody knows what they don't know. The quality score impact is attributed to clinical factors, not supply chain.
This is why the problem persists.
It's not that administrators don't care — it's that the data doesn't exist to make the case. Without visibility, there's no urgency.
Enter ICR: Instant Courier Rates
ICR — Instant Courier Rates — is the technology layer that makes delivery operations transparent, verifiable, and automatically reconciled from the moment a vehicle pulls up to the loading dock.
Here's what it actually does in a senior care context:
At the point of delivery, ICR captures a timestamped, digital proof of delivery — including photos, signature capture, and item-level scanning. Every box, every SKU, every quantity is logged against the original purchase order in real time.
This Is a Care Quality Issue, Not Just an Operations Issue
It's tempting to frame delivery efficiency as a back-office problem — interesting to the CFO, irrelevant to the DON. That framing is wrong.
When supplies arrive reliably, correctly, and verifiably, care teams spend more time on care.
Residents receive the right interventions on schedule. Families trust that the facility runs with precision. Staff feel supported rather than constantly firefighting logistics crises that aren't their job.
ICR doesn't just save money. It creates the operational foundation on which consistently excellent care is built.
The Bottom Line
The senior care industry is under relentless financial and regulatory pressure.
Margins are thin, staffing is challenging, and the expectations of residents and families have never been higher.
Every dollar lost to delivery inefficiency is a dollar that could fund a better dining program, a technology upgrade, or an additional care aide.
ICR closes that gap. Not with magic — with visibility, verification, and automation applied to a process that has been running on paper and goodwill for decades.
The cost of doing nothing isn't zero. It's $180,000 to $340,000 a year, compounding quietly, invisible on no single report, while your team works harder than they should have to.
The question isn't whether your facility can afford ICR. It's whether it can afford not to have it.
If this resonates, share it with an owner who needs to hear it. No demo script. No pressure. Just a real conversation. Get started today!
Share this post
Subscribe to ICR Newsletter
Home care logistics insights, delivery tips, and operational guides — free.
Unsubscribe anytime. We respect your inbox.
Need same-day delivery for your home care agency?
Instant Courier Rates provides medication pickup, pharmacy runs, and medical supply delivery across Atlanta and Gwinnett County. Get an instant quote →